Vestibular Rehabilitation
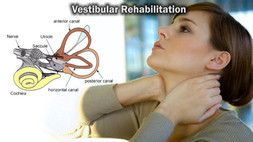
Vestibular hypofunction can be caused by various conditions, but ultimately leads to postural instability, visual blurring, and/or subjective complaints of imbalance. Evidence shows when vestibular rehabilitation is implemented the above impairments are reduced (Hall, 2009). Although details vary on what is included in vestibular rehab, some common elements include: vestibular adaptation and substitution exercises, balance and gait activities, and general conditioning (Hall, 2009). Common goals of vestibular rehabilitation include: VOR adaptation, habituation, sensory substitution, gait, posture, strength, flexibility, and endurance, all to maximize function (Alghadir, 2013). Activities
to increase tolerance of head and body movements are also incorporated
(Kaylie, 2012).
Adaptation:
Substitution:
Habituation:
Balance Exercises:
to increase tolerance of head and body movements are also incorporated
(Kaylie, 2012).
Adaptation:
- The remaining vestibular system adjusts its output according to the demands placed on it (Hall, 2009).
- The goal is long term changes to neural responses with reduction of symptoms (Hall, 2009).
- These exercises induce retinal slip, which assists in retraining Vestibular Ocular Reflex (VOR) function (Alghadir, 2013).
- Exercises involve head movements (vertical or horizontal) while maintaining focus on a target (Hall, 2009).
- Progressions include: increased velocity of head movements, movement of target and head, target placed in distracting visual field (Hall, 2009)
- VOR x1 - stationary object with head movements (Hall, 2009)
- VOR x2 - moving object with head movements (Hall, 2009)
- Exercises are progressed from sitting to standing, and finally to ambulation (Alghadir, 2013).
- Support surfaces are adjusted from firm to compliant as the patient progresses (Alghadir, 2013).
- Active movements are more effective then passive movements (Alghadir, 2013).
Substitution:
- The goal is to substitute alternative strategies for missing vestibular function (Hall, 2009).
- Potential substitution for the Vestibular Ocular Reflex (VOR) include the use of cervical ocular reflex, smooth pursuit, saccades, and central programming of eye movements (Hall, 2009).
- Potential substitutions for the vestibulospinal reflex includes the use of visual, somatosensory cues, or both to maintain stability (Hall, 2009).
- These exercises facilitate alternative strategies rather than teaching specific strategies (Hall, 2009).
- Programmed eye movements are used by directing the eyes to a target using large eye movements, before the head is turned towards the object (Hall, 2009).
- Saccade exercises are performed by shifting eyes quickly between targets up and down and left-to-right (Alghadir, 2013).
- Progression can be made from sitting to standing, and finally to ambulation (Alghadir, 2013).
- Substitution is used most commonly with bilateral vestibular involvement (Alghadir, 2013).
Habituation:
- This treatment is a type of mechanism of compensation (Hall, 2009).
- It includes long lasting attenuation of a response to a provocative stimulus brought about by repeated exposure (Hall, 2009).
- Systematic provocation of symptoms occurs by performing several repetitions of 2-3 movements or position changes that bring on the patient's symptoms (Hall, 2009).
- The systematic repetition leads to a reduction in symptoms and desensitization (Hall, 2009).
- It is more effective for peripheral causes of vertigo compared to central causes (Hall, 2009).
- This treatment is not recommended for bilateral involvement (Hall, 2009).
Balance Exercises:
- Static balance: trained under conditions of altered vision and somatosensation (Hall, 2009)
- Dynamic balance: Walking with head turns, quick turns to the right and left while walking, performing secondary tasks while walking such as tossing a ball, and performing cognitive tasks while walking (Hall, 2009)
- Progressions are made by narrowing the BOS and increasing the compliance of the surface (Hall, 2009).
- Walking programs are also prescribes, ideally outside and with an assistive device as needed for safety (Hall, 2009).
